Fifty isn’t what it used to be. Men today are running marathons in their 60s, building businesses in their 70s, and staying physically active well into the decades that earlier generations wrote off entirely. The science of aging has shifted dramatically, and there’s genuine reason for optimism. Still, reaching 50 does mark a biological turning point that quietly changes the rules of the game.
Beginning around age 50, a man’s body starts becoming more susceptible to ailments and disorders that can derail health, happiness, and even life itself. Most of these risks don’t announce themselves loudly. They build slowly, shaped by habits that once seemed harmless. The good news is that many of the most damaging patterns are completely within a man’s control to change.
1. Skipping Regular Medical Checkups
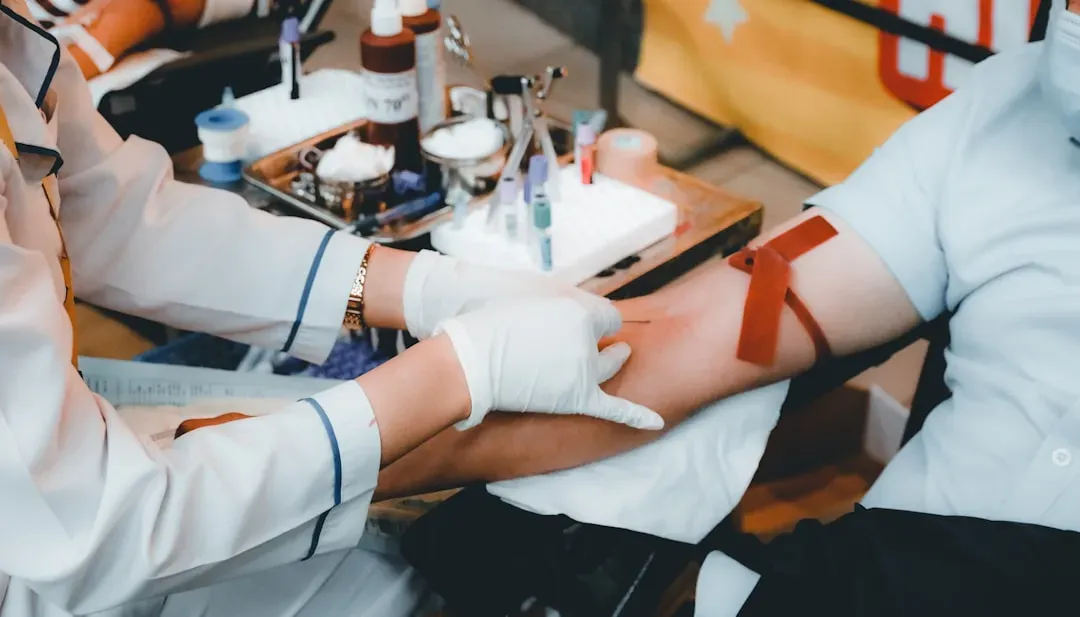
Surveys show that nearly half of men skip an annual physical exam, even though a regular checkup can reveal hidden health issues before they become serious problems. This tendency to avoid doctors, which many men carry confidently through their 30s and 40s, becomes genuinely risky after 50. The conditions most likely to threaten a man’s life at this stage rarely come with obvious warning signs until they’re well advanced.
Starting at age 50, most men should see their doctor each year for a checkup, particularly if they have any signs of cardiovascular disease, one of the two leading causes of death in men. The other is cancer. The U.S. Preventive Services Task Force recommends several key tests for people in their 40s and 50s, including annual blood pressure checks, cholesterol screening, Type 2 diabetes screening, and colonoscopy beginning at age 45 to detect colorectal cancer early. These aren’t optional extras. They’re the difference between catching something early and being blindsided by it.
2. Ignoring the Warning Signs of Belly Fat

After age 50, testosterone levels begin to dip, which causes changes in the way fat is distributed. Men might notice extra weight developing around their midsection. This shift isn’t just a cosmetic annoyance. Studies have found that spare tires trump even general obesity as a predictor of heart disease and diabetes. Visceral fat, the kind that accumulates deep around the organs, is metabolically active in ways that surface-level fat simply isn’t.
According to research published by the U.S. National Library of Medicine, men are more prone to develop visceral fat around the belly compared to pre-menopausal women. This visceral fat is incredibly dangerous and can increase the risk of a heart attack, type 2 diabetes, and other serious health problems. Ignoring a growing waistline after 50 isn’t just aesthetically unwise. It’s a compounding metabolic risk that grows more dangerous with every passing year of inaction.
3. Treating Strength Training as Optional

The progressive decrease in muscle mass begins once an individual reaches their 40s, and after the age of 50, muscle mass decreases yearly by one to two percent. Left unchecked, this loss of muscle, known as sarcopenia, carries consequences that go far beyond looking less toned. Sarcopenia is associated with a high risk of a wide range of adverse health outcomes, including falls and fractures, metabolic disorders, cognitive impairment, and mortality in general populations.
Among the exercise habits to prioritize in your 40s and 50s, along with endurance exercise, is resistance training, including exercises like squats, bicep curls, lunges, or push-ups where your muscles work against an external force. The U.S. Department of Health and Human Services recommends muscle-strengthening activities at least twice a week to maintain muscle mass and bone density. Most men default to cardio and skip the weights entirely. That’s the wrong trade-off at this stage of life.
4. Drinking More Than the Body Can Handle

To reduce the risk of alcohol-related harms, the 2020–2025 Dietary Guidelines for Americans recommends that adults who choose to drink should do so in moderation by limiting intake to two drinks or less for men on days when alcohol is consumed. After 50, the body processes alcohol less efficiently than it did at 30. The liver works harder, sleep is disrupted more easily, and the interaction between alcohol and common medications becomes a real concern.
Excessive alcohol and tobacco consumption increases the risk of a number of health issues, including cancer, heart disease, and stroke. Beyond the big-picture disease risks, heavy regular drinking in this decade accelerates cognitive decline and undermines the quality of sleep, which is already under pressure from age-related hormonal changes. Most people who drink don’t drink every day. That’s why it’s important to focus on the amount you drink on the days that you are drinking. Just because you didn’t drink all week doesn’t mean you’re in the clear to drink more on the weekend.
5. Letting Social Connections Quietly Disappear

Research has linked social isolation and loneliness to higher risks for a variety of physical and mental conditions, including high blood pressure, heart disease, obesity, a weakened immune system, anxiety, depression, cognitive decline, Alzheimer’s disease, and even death. For men, the 50s are often the decade when friendships start quietly unraveling. Careers plateau, children leave home, and the social scaffolding that was once built around work and family begins to thin out in ways that feel gradual until they don’t.
Meta-analyses have found that social isolation or loneliness in older adults is associated with a roughly fifty percent increased risk of developing dementia, a thirty percent increased risk of incident coronary artery disease or stroke, and a twenty-six percent increased risk of early mortality. According to a meta-analysis, lack of social connection heightens health risks as much as smoking fifteen cigarettes a day or having alcohol use disorder. Maintaining real human connection after 50 isn’t just emotionally rewarding. It’s a measurable health intervention.
6. Dismissing Mental Health as Someone Else’s Problem

Societal expectation and gender norms are damaging for men over 50. Older generations have been raised to be stoic and self-reliant, and mental health was viewed as taboo. Stress and anxiety is normal but, as we know, men are generally less likely to express their emotions or seek help for mental health problems. This silence has a cost. Depression may be common in older patients because of stressful or sad situations, like losing a loved one or transitioning from work to retirement. When a person’s depression interferes with daily life, it could be a medical condition that needs to be treated.
The cumulative impacts of earlier life experiences may start to come into play and impact mental wellbeing. Older men are also more likely to experience life events such as bereavement, a stalling career, drop in income causing financial worries, or reduced sense of purpose with retirement. Seeking support isn’t weakness at any age, but it takes on particular urgency after 50, when the combination of hormonal shifts, life transitions, and social changes can collide in ways that are genuinely destabilizing. For many men, career, financial, and family pressures can make the 50s a very stressful time. Stress is a known risk factor for heart disease. Recognizing that and doing something about it is simply good judgment.
The habits that shaped the first fifty years don’t automatically serve the next fifty. Some of them need to be retired, not because aging demands retreat, but because the second half of life rewards a different kind of attention. The choices you make in your 40s and 50s have an outsized impact on your quality of life in your 60s, 70s, and beyond. You still have plenty of time to slow the aging process and keep preventable health problems at bay.





Leave a Reply